OCD is capable of making the smallest thing into the biggest tragedy. This type of distorted thinking is called catastrophizing. My brain is very good at making a simple to-do list the most stressful event I have ever faced. That's why when it began time to pack for a few months of treatment in Wisconsin, I panicked. The idea of packing so much was brutal, but with the help of my family, I got through it. I was just trying to survive without a breakdown at that point. I spent the day before leaving for Rogers with my mom. We went shopping and went to Olive Garden (aka the best place on Earth). We had a wonderful day and then it came time to say goodbye to Jake and my friends. There were tears. I remember driving home from saying goodbye to Jake and I was sobbing and banging on the steering wheel. Nothing seemed fair. Why did I have to worry all the time about everything and the simplest task seemed impossible? Why did no one else face these struggles? I would soon find out that I wasn't alone.
The next morning I said goodbye to Raegan, my three-year-old sister and Sydni my now thirteen-year-old sister. Raegan believed that I was going to camp and I would be back soon. It was absolutely heartbreaking saying goodbye.
The road trip was long, but I was amazed at the beauty of Rogers Memorial Hospital when I arrived in Oconomowoc, Wisconsin. The hospital has the most beautiful garden I've ever seen and it was surrounded by lakes. I felt welcomed there. The admission process was long because it took absolutely forever for our insurance to go through. We waited in the lobby of the main hospital building for hours. I just wanted to get the process going. When we finally heard from the insurance, I went up to a room in the Child and Adolescent Center(which was a whole separate building) and I met my entire treatment team. My treatment team consisted of my therapist Julie, my psychiatrist Dr.Lake, my teacher Jane, and my behavior specialist Alyssa. Then it came time to head down to my unit to meet everyone that lived on CAC West(one of the two units for adolescents in the CAC).
The first person to greet me was in fact the best friend I would meet at Rogers. It was Rachel, my first roommate. She was so welcoming and completely didn't mind when I asked her so many questions. We got along right from the start and it was then talking to her that evening when I realized it wouldn't be so bad there after all. That first "real talk," as she would call a deep conversation, opened my eyes to how OCD differs from person to person, but there is hope for everyone who has it. My nerves went away almost completely and my confidence boosted. I could do it.
The next day I discovered I weighed eight pounds more than I did when I weighed myself a few months earlier. I had quit stepping on the scale when I began to weigh myself multiple times a day. The obsession with weight and the compulsion of weighing myself had gotten out of hand. I also had a problem with binge eating due to stress, so the eight pounds were definitely justified. I remember trying not to freak out at the weight gain. I felt panicked. I asked Dr.Lake to write an order to meet with Tricia, the dietician within the next few days. Later that day, I was also introduced to Jenna, my group therapist. Most kids at Rogers have the same person as their primary therapist and their group therapist, but since my therapist Julie worked part-time and only had a few people on her caseload, I would be working with Jenna for group therapy each day. Heather, my new behavior specialist, was also introduced to me the second day. Heather began working with me because Alyssa had to work with someone else.
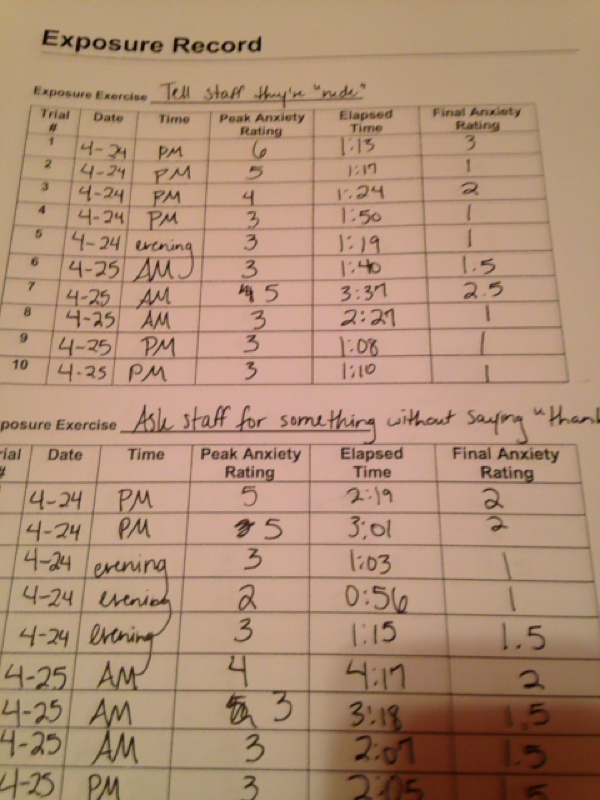
The next few weeks all consisted of lots of treatment work. The type of therapy Rogers uses to treat OCD is called exposure response prevention(a type of cognitive behavioral therapy). It deals with doing the things that make you anxious, so you can get used to them over time. ERP is the most effective type of therapy for OCD according to many specialists. I got five exposures, or assigned behaviors that will produce anxiety, to start with. Exposures work by doing the action, starting your timer, marking your peak anxiety(on a scale of 1-7), waiting until your anxiety cuts in half, stopping the timer, and marking your final anxiety. Over time your peak anxiety will drop. Once your peak anxiety is at a two or lower, you can move on to a new exposure and that exposure would be completed. You did five trials of each exposure each day(at least 25 trials total each day). I also got a ban book. My first bans were mental reviewing(going over my to-do list over and over in my head), checking(looking to see if I did something correctly), and reassurance seeking. Each time I submit to a ban, I would mark a submit for that day and the same went for resists for each ban.
Each weekday consisted of the following schedule:
Breakfast at 8:00 AM
School 8:30-9:30/8:30-10:30
Experiential Therapy/Art Therapy until noon
Lunch at noon
Group Therapy 12:30-1:30
CBT 1:45-4:45
Dinner 5:00
Group Check-in (everyone on the unit checks in with a resident counselor about how they are feeling emotionally and physically) at 5:30
CBT 6:00-7:00
Free time 7:00-9:30
The busy schedule took a long time to get used to. I was very tired and stressed a lot of the time for the first few weeks. I still struggled to wrap my head around keeping up with school and treatment work even though it was required that the school make accommodations for me since I was being hospitalized. School was still the biggest stressor even with being in another state. College Writing stressed me out to the core and I did my best to make it through.
While the four hours of treatment work each day was incredibly intense, the CAC was still lively and fun. We went on group outings to the movie theatre, the bookstore, the ice cream shop, or the hobby store every weekend. It was so nice to get out and about after being stuck in the same place all week. Rachel and I would also paint our nails on the weekends since the weekend was packed with downtime. My favorite pass time thought was playing Just Dance with one of my guy friends on the unit. It was always a blast!
Exposures were especially tough to do at first. The idea of sitting down for four hours and confronting my fears was scary. I remember having the exposure of telling a staff member that they were rude and just freaking out. I know that the exposure itself may sound extreme, but the over-correction helps you normalize your thoughts. Most of my exposures had to do with not people pleasing, looking at examples of bad hygiene(ex: looking at a picture of long fingernails), and thinking about natural disasters at first. I also had to put many different sticky substances on my hands.
I talked to Jake and my family every night. I would update them and rush through my calls. Calling home was just another thing on my mental to-do list. It would stress me out, so I would just call them and give them a brief summary of my day and get it over with. This would be fixed later.
By Day 14, I began interoceptives(exposures that replicate the physical symptoms of a panic attack). They would eventually help me have less severe panic attacks whenever I relapsed and yes, RELAPSE HAPPENS TO EVERYONE NO MATTER WHAT! That was an extremely hard lesson to learn. Relapses will happen, but you just have to jump back on track. I also discovered that my behavior specialist, the one that handles all of my CBT work, was leaving my unit and that my new BS would be Lindsay. I was a little nervous, but I knew Heather would leave me in good hands when she did leave.
We did so many amazing things in ET(experiential therapy) that I always looked forward to it. The most unique thing in those first few weeks was definitely going to the gas station petting zoo for someone's discharge ET session. It was a legitimate petting zoo for being at a gas station! I also enjoyed the ropes course a lot.
Julie introduced me to mindfulness(a practice that brings your focus back to the present moment when you are worrying about the future or the past) a few weeks into my stay. It completely changed my life. I was learning to use meditation and the idea of being present to lessen my anxiety all on my own.
Around Day 23, I was put on an individualized meal plan by Tricia the dietician to help me face the all-or-nothing attitude I had towards food. It helped me begin to learn about healthy portion sizes and the need for all food groups in a meal.
One of the worst parts of my first weeks at Rogers was when Dr.Lake began to ween me off of some medications I was on. He wanted me off of some of the medications I was on because they proved to be physiologically addictive. I began to have withdrawal symptoms when he began weening me off of one medication. I had headaches and chest pains constantly. The pain lasted for about a week. I had never been so upset with him before then.
I felt like I was in a culture shock going to Rogers Memorial Hospital, but my journey was just beginning and with all the amazing support that I had and the fantastic friends I was making, I was unstoppable.
 RSS Feed
RSS Feed
